In an effort to produce some information regarding why those two recent NPR articles (A and B) are the exact opposite of what we’re attempting to convey to our audience and the women we work with, Dr. Mathews asked if I would help construct a response. I started writing, but then realized I’d basically already completed this task. Below you will find the Appendix from my first book, The First Trimester, which I dedicated to discussing diastasis.
Diastasis Rectus Abdominis (DRA)
While not exactly part of my day-to-day experience of the first trimester of pregnancy, I deal with diastasis rectus abdominis (DRA) with patients and the moms in my BIRTHFIT courses on a regular basis. I also couldn’t write a book without at least addressing it. I talked about it a few times throughout the book, so for those of you looking for more information, here it is.
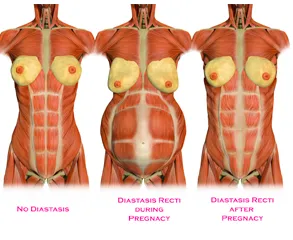
I first heard about DRA from a Dynamic Neuromuscular Stabilization course in 2009. It actually had nothing to do with pregnancy, but was demonstrated via videos regarding poor loading techniques in those with Cerebral Palsy or simply folks who could not effectively manage their own intra-abdominal pressure system. DRA is a stretching of the connective tissue that holds the two rectus abdominis (six-pack) muscles together; it occurs from repetitively using poor loading techniques (not stabilizing your body when lifting an object), but also in rapid expansion of the abdominal tissues, as is consistent with pregnancy. There are some thoughts on how to prevent/correct/heal DRA, but there isn’t a lot of consistency if you scour the interwebs. Some say to do planks, others say avoid them completely. Some say pull your belly button toward your spine, others say don’t EVER do that. Some say this, others say that, etc. It can be hard to sift through the info, especially when you’re a new mom. Since I’ve been studying DRA for several years, I’ve learned quite a bit about it, and have seen which methods work and which have been less than ideal in implementation. While some of this will be a little science-heavy, I’ll try to keep it relatively concise.
To keep things simple: if the diaphragm is not stacked on top of the pelvic floor in all postures, then the body is set up for some amount of dysfunction. This occurs when posture isn’t ideal, but also when a person sucks in their stomach or holds tension in their abdomen. This prevents ideal diaphragmatic breathing, wherein the diaphragm lowers and the abdomen expands 360 degrees, which would set the diaphragm on top of the pelvic floor easily. This is unfortunately where most fitness programs regarding DRA are currently failing. They’re missing the big picture when it comes to stability of the torso being established by the diaphragm.
In the ideal breathing and postural pattern, the abdomen is solid and stable without having excess tension of the musculature. Stability is created by the diaphragm. The diaphragm rests parallel to the pelvic floor (relatively speaking considering both are rounded structures), which gives an almost piston-like stabilization of downward motion of the diaphragm resulting in eccentric activation of the pelvic floor. (Eccentric contraction means a muscle is lengthening under load rather than shortening, as it does in concentric contraction. An example would be in a typical bicep curl: bringing the weight towards your body would concentrically activate the bicep; lowering the weight would eccentrically activate the bicep.) With this type of breathing, intra-abdominal pressure (IAP) creates a stable environment and the transversus abdominis muscle (TrA) gets some eccentric contraction with every breath. Most programs are encouraging participants to concentrically activate TrA, which destabilizes the IAP system (1).
I see coaches and other healthcare professionals posting on their social media accounts and blogs about engaging the TrA by pulling them in, specifically during pregnancy. Not only is this blatantly wrong and ill-advised regarding everyday life stabilization, it’s terrible during pregnancy. A patient sent me a video she saw on Instagram with the caption, “Is this a no-no?” A pregnancy/postpartum-specific coaching program showed a pregnant mom sitting on a kinesio ball actively sucking her belly in, then releasing and repeating it with some arm movements. The coach had written about using the pulling in motion to “hug” the abs together in an effort to stabilize the midsection, and how important this was during pregnancy. I responded to my patient that it was definitely a no-no, and congratulated her for recognizing a bad movement pattern despite lots of attention on social media. A cursory look through the account showed me pregnant women doing crunches as well, and was enough for me to send my patient another message, encouraging her to unfollow that account.
So why is that advice so bad? Several reasons come to mind, actually. First, it’s based on flawed research that’s incredibly outdated. Second, it doesn’t allow for proper use of the diaphragm. Third is that it actually contributes to poor loading techniques of the entire abdomen, which can lead to (or worsen) a diastasis. DRA has very recently become this buzzword that nearly every coach, yogi, fitness professional, PT, or chiropractor who works with women is talking about. Unfortunately, most of them don’t have great information, and they’re spreading around the bad info like wildfire.
Why doesn’t everyone agree? Why are there such strong differing opinions regarding how to create stability and how to decrease DRA? In comes the outdated research. A 1999 study by Hodges and Richardson (well-respected within medical and manual therapy circles) concluded that in subjects with low back pain, they did not activate TrA as quickly as those without low back pain. The conclusion was drawn that we therefore must train people to activate TrA in an effort to decrease low back pain (2). But the opposite was true. Subjects were trained to activate TrA prior to loading their spine, but they still had low back pain. People obviously got better at activating TrA, but still couldn’t functionally stabilize, because they’d simply isolated one muscle in a broken series. Further studies have gone on to show that multiple muscles do not engage properly in those with low back pain (3). This is because the body works as a unit, made up of many parts that need to function together. If one or more parts isn’t working, the entire system falters (4). Fixing the individual muscles doesn’t actually fix the system.
A little more science-y stuff for you nerds to salivate on: statistics show that 30-70% of all pregnant women will have some amount of diastasis; it’s practically considered a normal variant of pregnancy (5). However, what’s NOT normal is when the diastasis stays beyond 8 weeks postpartum, which can occur in as high as 60% of cases (5). Unfortunately, many health professionals completely disagree about what to do with this separation. Surgical intervention is risky, and doesn’t boast superior outcomes to conservative treatment in the literature. A large part of that is because there isn’t a ton of literature on the subject. Randomised Controlled Trials (RCTs) are the gold standard in research. This type of study means that no one participating in the clinical trial has a dog in the fight – everyone is strictly in it for the information being obtained, and not to prove a point. No one knows if they’re giving a placebo or receiving a placebo; everyone is blind to all parts except their own participation. These types of trials are hard to come by, but they give the most accurate information available. A systematic review takes available studies and makes correlations based on review of all the literature. If a systematic review consists of RCTs, then you’re getting a synopsis of the best info out there. Typically, systematic reviews will also include literature such as case studies and less controlled versions of clinical trials. Now that you have a little background on what types of literature is available, here is the conclusion drawn from a systematic review in 2014 in the Journal of Physiotherapy: “Based on the available evidence and quality of this evidence, non-specific exercise may or may not help to prevent or reduce DRAM during the ante- and postnatal periods” (6). It doesn’t sound too promising, does it? There’s junky information out there, and no studies seem to come to any obvious conclusions. Non-specific exercise may help, but it may not. And one of the most common things that practicing clinicians can agree upon is that DRA contributes to various ailments such as low back pain, urinary incontinence, or pelvic pain. But a study from 2015 showed that there was no correlation between women with DRA and a higher incidence of lumbopelvic pain (7).
So if the evidence is inconclusive, and more research needs to be done, then where do we go from there? Well, my vote is to go where the research is sound. While it doesn’t have anything specifically to do with pregnancy or postpartum, there is a decent amount of research coming out of the Prague School regarding the use of Dynamic Neuromuscular Stabilization and improving the functionality of the core. The exercises in the studies are all based on developmental kinesiology (something else that’s been studied immensely), which means they’re based on how babies learn to move. You know what babies have? Relaxed muscles, no low back pain, and a stable midsection (after they’re 4.5 months old). What the studies conducted by those implementing DNS have discovered is that those without a properly functioning diaphragm have aberrant movement patterns and present with low back pain (8). They’ve also discovered that the diaphragm doesn’t just function in breathing, but also plays a huge role in stabilization of the trunk (1). And they’ve discovered that improving the stabilization and respiratory function of the diaphragm leads to improvement throughout the body (9). Given this information, I start all of my patients with simple breathing exercises. Getting their breath out of their chest and into their abdomen requires that they relax their belly. This is easier for pregnant women, but much harder for postpartum women to do. Relaxing your belly means you can’t suck it in anymore. This means that people can actually see the extra weight you’re attempting to hide, which is a hard thing for a lot of people to do. But it’s the only way to fully utilize the diaphragm, which is the beginning of stabilizing the abdominal system.
Additionally, I give women (and men, because you’d be surprised how many men are walking around with DRA and don’t know it until they come into my office) exercises similar to movements you’d see a 7.5 month old baby doing – stabilizing on their side and beginning to move toward turning. (For a great example, go to BIRTHFIT’s YouTube channel and check out Dr. Erica Boland doing the Functional Progression exercises – that’s the same Erica I’ve mentioned throughout the book, so you know she’s awesome.)
The hardest thing for people to do is to let tension go from their belly. But that’s the fastest way to begin to stabilize the midsection, which is unstable in the event of DRA. It allows you to naturally stack your diaphragm on top of your pelvic floor, which gives you a stable base as well as naturally better posture. This is also a great starting point for improving pelvic floor awareness and function. Maybe my next book will be all about the pelvic floor.
Lindsay Mumma, DC
BIRTHFIT NC Regional Director
Citations
(1) Kolar P, Sulc J, Kyncl M, Sanda J, Neuwirth J, Bokarius AV, Kriz J, Kobesova A.
Stabilizing function of the diaphragm: dynamic MRI and synchronized spirometric assessment, J Appl Physiol. , 2012;42(4):352-62
(2) PW Hodges and CA Richardson. “Altered trunk muscle recruitment in people with low back pain with upper limb movement at different speeds.” Archives of physical medicine and rehabilitation 80 (1999): 1005-1012. http://www.ncbi.nlm.nih.gov/pubmed/10489000
(3) Stuart McGill, “Laying the Foundation – Why we need a different approach,” Ultimate Back Fitness and Performance, ed. Stuart McGill, 9-27. Canada: Wabuno Publishers, Backfitpro Inc, 2004.
(4) Dionne, C. “How Are We Still Getting It Wrong: Abdominal Hollowing vs. Bracing”. Breaking Muscle. Accessed 4/27/15. http://breakingmuscle.com/mobility-recovery/how-are-we-still-getting-it-wrong-abdominal-hollowing-vs-bracing
(5) Kimmich N1, Haslinger C, Kreft M, Zimmermann R.[Diastasis Recti Abdominis and Pregnancy]. Praxis (Bern 1994). 2015 Jul 22;104(15):803-6. doi: 10.1024/1661-8157/a002075. [Article in German]
(6) Benjamin DR, van de Water AT, Peiris CL.Effects of exercise on diastasis of the rectus abdominis muscle in the antenatal and postnatal periods: a systematic review. Physiotherapy. 2014 Mar;100(1):1-8. doi: 10.1016/j.physio.2013.08.005. Epub 2013 Oct 5.
(7) Fernandes da Mota PG, Pascoal AG, Carita AI, Bø K. Prevalence and risk factors of diastasis recti abdominis from late pregnancy to 6 months postpartum, and relationship with lumbo-pelvic pain. Man Ther. 2015 Feb;20(1):200-5. doi: 10.1016/j.math.2014.09.002. Epub 2014 Sep 19.
(8) Kolar P, Sulc J, Kyncl M, Sanda J, Cakrt O, Andel R, Kumagai K, Kobesova A.
Postural Function of the Diaphragm in Persons With and Without Chronic Low Back Pain. , J Orthop Sports Phys Ther, 2012;42:352-362, Full text displayed with permission of the Journal of Orthopaedic and Sports Physical Therapy, and the Sports Physical Therapy Section and the Orthopaedic Section of the American Physical Therapy Association.
(9) Kobesova A, Dzvonik J, Kolar P, Sardina A, Andel R.
Effects of shoulder girdle dynamic stabilization exercise on hand muscle strength. , Isokinetics and exercise Science. , 2015;23:21-32, 0959-3020
Get Started
Effective programs for both MIND ⊕ BODY
This is a general strength and conditioning program for women in all seasons and cycles of life. You receive four workouts each week with options for those with limited equipment and variations on movements.
Start moving and training with your cycle ❤︎
Slow is Fast when you heal your core and pelvic floor from the inside out by starting with breath work, natural movement patterns, and continue to progressively build upon a solid foundation. The number one referral for doctors and midwives.
Are you open to conception? Join us in B! Community training. A general strength and conditioning for women that train while honoring their menstrual cycle. Everyone is in a different part of their journey, we support you where you are.
Do Pregnancy Different, when you connect with your body daily through a safe, effective prenatal training program for all levels and all fitness backgrounds that includes core and pelvic floor prehab, mobility, strength, and conditioning.